Covid in Sheffield: Staff absences at Sheffield Teaching Hospital due to coronavirus rise by 40%
and live on Freeview channel 276
New figures show the number of NHS hospital staff off across England has doubled on average since the start of December.
Some 2,093 staff at Sheffield Teaching Hospital – which employs 17,000 people – were ill with coronavirus or having to self-isolate on Boxing Day, up 23 per cent from 1,699 a week earlier and up 40 per cent up from 1,485 at the start of the month.
Advertisement
Hide AdAdvertisement
Hide AdThe city’s other NHS hospital, Sheffield Children’s Hospital – which employs 3,000 people – saw a rise in Covid-related absences of 12 per cent, from 305 at the beginning of the month to 347 on Boxing Day.


The NHS England figures come as new Office for National Statistics (ONS) data also showed an estimated 2.3 million people across the UK had Covid-19 during the week ending December 23.
This is up from 1.4 million in the week to December 16 and the highest number since comparable figures began in autumn 2020.
Meanwhile, separate figures showed that the number of Covid patients in hospitals across England had climbed to 11,452 on Thursday, which is the highest level since February 26.
Advertisement
Hide AdAdvertisement
Hide Ad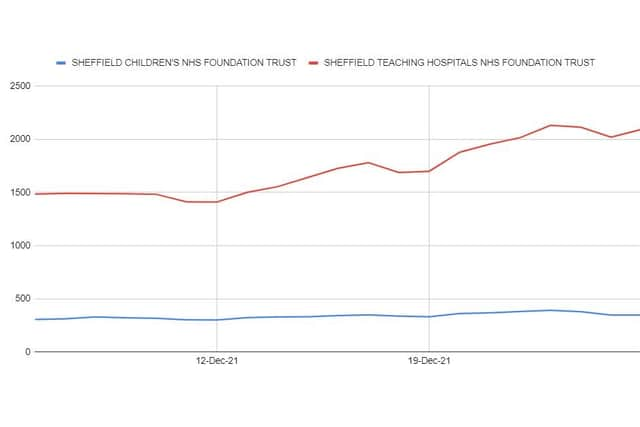

Matthew Taylor, chief executive of the NHS Confederation, said the NHS is facing a “perfect storm” of rising Covid hospital admissions and illness alongside increasing numbers of frontline workers being off sick.
“The NHS is putting in plans to step up once again for patients with the new Nightingale surge hubs, extra support from community services and virtual wards, but there is no doubt the whole system is running hot,” he said.
“While the Government seems determined not to increase restrictions in England, it is vital we all behave in ways that will not exacerbate an already dangerous situation.”

The scale of rising staff absences has led to political calls for an emergency Government Cobra meeting to be convened “without delay” by the Prime Minister to “thrash out a comprehensive rescue plan”.
Advertisement
Hide AdAdvertisement
Hide AdLiberal Democrat health spokeswoman Daisy Cooper said the health service was being “stretched to breaking point”, adding: “Our NHS is in desperate need of support. The Government must give this crisis the attention it deserves.”
NHS England national medical director Professor Stephen Powis said the health service is setting up the Nightingale surge hubs at hospitals across the country and recruiting thousands of nurses and reservists.
He added: “We don’t yet know the full scale of rising Omicron cases and how this will affect people needing NHS treatment but, having hit a 10-month high for the number of patients in hospital with Covid while wrestling with sharply increasing staff absences, we are doing everything possible to free up beds and get people home to their loved ones – and in the last week hundreds more beds were freed up each day compared to the week before.
“The NHS is on a war footing, and, while staff remain braced for the worst, with Covid absence for NHS staff almost doubling in the past fortnight, keeping as many colleagues as possible at work on the front line and minimising absence, will be essential in the next few weeks.”
Advertisement
Hide AdAdvertisement
Hide AdMeanwhile, ministers have been warned they must be ready to apply restrictions “at pace” as the NHS puts itself on an emergency footing to deal with a possible surge in Covid-19 patients.
Chris Hopson, chief executive of NHS Providers, said trust leaders recognise that the UK Government’s threshold for introducing extra measures in England “hasn’t been crossed yet” but that additional capacity is being created in case hospital pressures increase.
Government data shows the number of coronavirus patients in UK hospitals jumped by 44 per cent week on week to 11,898 on Wednesday, the highest number since March 2.
In Scotland and Wales, nightclubs are closed to New Year’s Eve partygoers, and restrictions have been placed on hospitality.
Advertisement
Hide AdAdvertisement
Hide AdBut in England, ministers have opted to forgo measures beyond the UK Government’s Plan B, which includes mandatory Covid passes for large events, increased mask-wearing in public places and work from home guidance.
Mr Hopson, chief executive of the group which represents health trusts in England, said even if extra restrictions are put in place to control the Omicron variant, it will take two weeks to reduce the hospital admission rate.
He told BBC Radio 4’s Today programme: “It is the Government who sets the rules on restrictions, not the NHS, and we know that the Government has set a high threshold on introducing new restrictions.
“So, on that basis, trust leaders can see why the Government is arguing that, in the absence of a surge of seriously ill older patients coming into hospital, that threshold hasn’t yet been crossed.
Advertisement
Hide AdAdvertisement
Hide Ad“But we still don’t know if a surge will come, and indeed we are exactly talking about the preparations we are making for that surge right now.
“So, in terms of restrictions, I think we are in exactly the same place we’ve been for the past fortnight, which is the Government needs to be ready to introduce tighter restrictions at real speed should they be needed.”
The Nightingale hubs are being established at some hospitals to deal with a “super-surge” in Covid patients in a move that Mr Hopson said would require the NHS to “go into an emergency mode” amid staff shortages, partly due to high coronavirus infections.
He said recently retired health workers and volunteers would be asked to staff the hubs, which would be used for patients “who are effectively over the worst” and being readied for discharge.
Comment Guidelines
National World encourages reader discussion on our stories. User feedback, insights and back-and-forth exchanges add a rich layer of context to reporting. Please review our Community Guidelines before commenting.

