Sheffield Teaching Hospital: 'Significant improvements' needed as staffing shortages impact patient safety
and live on Freeview channel 276
Sheffield Teaching Hospitals NHS Foundation Trust has been ordered to make “significant improvements” by the Care Quality Commission following an unannounced inspection in October and November.
The scathing report has dropped the healthcare provider from its ‘Good’ rating in 2018 to ‘Requires Improvement’ in all areas – except for its ability to keep patients safe, which has been graded ‘Inadequate’.


Advertisement
Hide AdAdvertisement
Hide AdTrust bosses said they are “devastated” by the findings, vowed to make change, and said 500 more nurses have now been recruited.
The visit last year took in wards from Northern General Hospital, Royal Hallamshire Hospital, Jessop Wing and Beech Hill Assessment and Rehabilitation Unit.
Severe staffing problems across the Trust, a lack of proper support for patients with mental health problems and poor medical care at Royal Hallamshire Hospital all contributed to downgraded rating.
But most damning is the findings around the Trust’s maternity service, which, despite being rated inadequate with severe safety concerns in March 2021, was found to be in some cases even worse during the visit in autumn just a few months later.


Advertisement
Hide AdAdvertisement
Hide Ad“We re-inspected the maternity services as part of this inspection and found there was little or no improvement to the quality of care patients received, in some areas the service had deteriorated further,” the report reads.
“For example, there was significant concerns about the assessment of patients in the labour ward assessment unit, maternity staffing and delays in induction of labour.”
Further, the CQC’s deputy chief inspector for the north, Ann Ford, said: “It was most disappointing that several areas which we have identified in the last 12 months as needing urgent improvement had still not been fully addressed...Our inspectors found deterioration, as well as safety concerns in maternity.”
The report deals another blow to Sheffield’s healthcare Trust, which received an inadequate rating and emergency measures were put in place in June last year after the Jessop Wing, which was once rated outstanding, was downgraded.
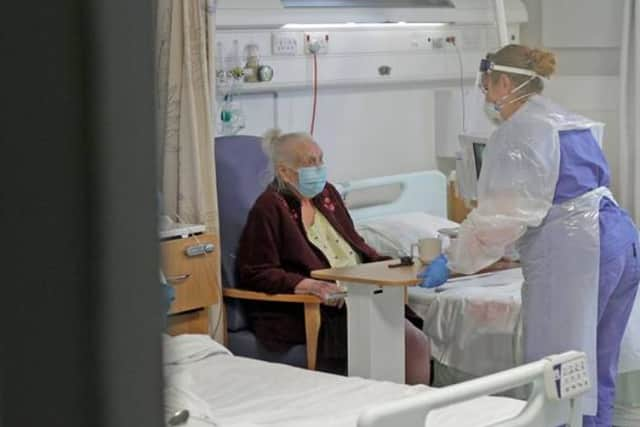

Staffing numbers was a key issue in nearly all areas.
Advertisement
Hide AdAdvertisement
Hide AdThe Trust claims it was suffering from severe staff sickness rates during the inspection, and the report does highlight that staff “treated patients with compassion and kindness”, while consistently reporting they were “proud to work for the Trust”.
However, it did not reflect kindly on patient safety.
Despite having enough medical staff to keep patients safe, the overall staffing levels were a repeat concern.
“The Trust did not have enough staff to care for patients and keep them safe,” the report reads.
“Staff were not always up to date with training in key skills. The Trust did not always control infection risk well. Staff did not always assess risks to patients, however, when they did, they did not always act on them.
Advertisement
Hide AdAdvertisement
Hide Ad“Staff did not always provide good care and treatment…Staff worked together for the benefit of patients, but they did not advise them on how to lead healthier lives.”
Concerns were also raised over mental health support across the Trust, citing: “The failure to provide safe and appropriate care to patients with mental health needs had resulted in incidents of avoidable harm.”
‘Medical care’ was also rated inadequate in all areas at Royal Hallamshire, with noted failings in infection control, cleanliness, and in how wards were designed and maintained to keep patients safe, for example with substances not being stored correctly or how rooms with hazardous substances were not locked. Again, inspectors noted that “most wards we visited” at Royal Hallamshire were short staffed.
“Staff said that wards were often left unsafe and even if their ward was fully staffed, staff would then be moved to another ward to make up short staffing numbers on that other ward...they felt they were made to just get on with it if staffing wasn’t available,” the inspector wrote.
Advertisement
Hide AdAdvertisement
Hide AdMs Ford added: “I recognise the enormous pressure NHS services are under across the country, especially in urgent and emergency care, however it’s vital that senior leaders are visible and have good oversight to manage and mitigate.
“It was evident that some staff were being demoralised when raising concerns to improve patient care…A number of staff told us they had stopped reporting incidents and when they did, the Trust response was slow and untimely so reduced opportunities for timely intervention
“Senior leaders must do more to support staff and create a no blame culture of reporting, learning and continuous improvement as well as a culture of openness and transparency. This must be addressed as a matter of urgency.
“We were however pleased to hear that most staff were proud to work for the Trust and overall had a commitment to providing good care and positive experiences for patients, often under demanding and challenging circumstances.”
Advertisement
Hide AdAdvertisement
Hide AdThe Trust was provided feedback immediately after the inspection, which provided an action plan and is being supported by NHS England and NHS Improvement.
Chief executive Kirsten Major said: “Everyone in the Trust has given their all during the past two years to manage the demands of the pandemic and we are determined to address the issues raised in this report with the same commitment.
“I want to assure our patients that our top priority will always be to do our very best for everyone who needs our care.
“We have had less staff at times including when the inspection took place because of high staff COVID sickness and there is no doubt that some of our normal ways of working or delivering care suffered because of the focus we had to have on dealing with the immediate crisis in front of us at the same time as continuing to deliver emergency and cancer care plus as many planned operations as we could and leading the vaccination programme for South Yorkshire.”
Comment Guidelines
National World encourages reader discussion on our stories. User feedback, insights and back-and-forth exchanges add a rich layer of context to reporting. Please review our Community Guidelines before commenting.

