How busy is your GP Sheffield: a day with Birley Health Centre doctors and patients
and live on Freeview channel 276
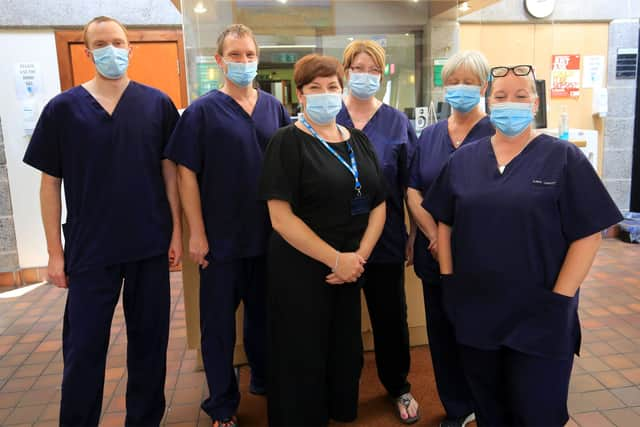
On Friday (November 5), The Star visited Birley Health Centre in Sheffield, to spend the day with Dr Ben Allen and the rest of the staff there and see first hand what the job of a GP is like at the moment.
A reporter sat in with Dr Allen to witness the day-to-day running of the surgery, and it quickly became apparent that the often-spread stories about it being more difficult to get face-to-face appointments are not true, while underfunding and increasing demand remains a significant difficulty for the NHS.
How busy are GPs?

Advertisement
Hide AdAdvertisement
Hide AdOn the day The Star visited Birley Health Centre, Dr Ben Allen said that they expected to see around 124 patients. The capacity of the health centre, based on the number of staff they have available, is 100.
The health centre was fully staffed that day, with five doctors and two PAs working. This means 100 is the maximum capacity at Birley on any given day - which Dr Allen describes as the amount GPs can ‘comfortably see’.
However, the number of patients seen is consistently far higher than that - a sign of the NHS being overstretched that Dr Allen said is ‘typical’ of most GP surgeries in Sheffield.


On most days, the surgery sees around 50 more patients than it has capacity for, with Monday usually being the busiest day where around 27 per cent of the week’s patients are seen, which equates to 220 appointments.
On other days, Dr Allen says the average is about 150.
Advertisement
Hide AdAdvertisement
Hide AdBy 8.30am on Friday, 17 patients had already been seen at the surgery.
On top of the 124 appointments expected to be carried out by Birley Health Centre staff that day, the staff also had to deal with 60 blood tests and as many as 300 prescriptions.
GP staff must also handle the letters that come in from other health services such as A&E, hospitals and mental health services, which ask them to see more patients, and any number of ‘tasks’ that come in, which can include jobs related to the day-to-day running of the surgery. Then there are the home visits to carry out.
Dr Allen estimated that on average he works 11-hour days, and he said that a typical day involves 15 abnormal blood tests, seven letters needing actions, 300 prescription requests, 40 new appointment requests, 20 to 40 electronic clinical queries from other medical staff, support for three to five junior colleagues and a home visit.
Advertisement
Hide AdAdvertisement
Hide AdWith this level of demand, it is inevitable that GPs are unable to see every single patient face-to-face, for as long as the patient wants, regardless of the condition.
Are patients not being given face-to-face appointments?
In spite of this huge workload, and the limited time in which the work must be done in order to avoid waiting lists building up, GPs have come under criticism over the perceived ‘difficulty’ in getting a face-to-face appointment.
The Government announced £250m extra funding to enable more face-to-face appointments. Doctors criticised this approach as ‘not enough’ to make a difference and branded the ‘obsession’ with face-to-face sppointments as ‘dangerous’ and claims that patients can’t get when they need them as false.
The Star has seen the data for the patient appointment requests that have come into Birley Health Centre over the past eight weeks, which shows that in fact more patients are being seen face-to-face than the number who request that treatment.
Advertisement
Hide AdAdvertisement
Hide AdSince September 13, around eight per cent of patients who requested an appointment at Birley asked for a face-to-face meeting with a medical professional.
Meanwhile, 56 per cent requested an appointment over the phone, and 36 per cent asked for help to be sent via email.
What actually happened over those eight weeks was that on each day since September 13 between 15 and 26 per cent of patients who requested appointments have been seen face-to-face.
And on any given day between 30 and 40 per cent of patients were dealt with over the phone or by email.
Advertisement
Hide AdAdvertisement
Hide AdDr Allen explained: “Email can be an efficient and safe way to help somebody, but there will be some patients who need face-to-face. And in some cases, a patient will ask for a phone call or an email and we will tell them that they need to come in.
“More important than efficiency, though, is helping people using the right method. It is not efficient to get it wrong.
“Equally, it is important not to give sombody a face-to-face appointment who does not need it, so we say we will call them instead. In those cases, we may not be giving one person exactly what they want, but in doing that we ensure we have the time to give a number of other people what they need.”
Examples given today include a two-month-old baby with a cough and wheezing, whose family asked for an email appointment. Dr Allen has instead asked them to attend a face-to-face appointment. Another was somebody who wanted to be seen face-to-face for athlete’s foot, who was instead told to go and see a pharmacist.
Advertisement
Hide AdAdvertisement
Hide AdDr Allen added: “We will always do what is needed. If we just let the first patients who rang up have a face-to-face appointment then we would only see half the people that we manage to see this way.
“We also try to see everybody on the day they ask to be seen. If somebody gets in touch with us between 8am and 1pm they will almost certainly be seen to that day. And if they get in touch after that and it is urgent we will try and see to them, too.”
Why might you be sent to somebody other than a GP?
Another criticism often levelled at GPs is down to the fact that patients expect to be seen by a doctor, and in order to meet demand it is not always the most suitable thing to happen.
Nowadays, a ‘triage’ system is in place which means that a patient’s condition is reviewed and then they are sent to the most appropriate medical professional. This system prevents doctors’ time being spent treating things that another trained professional – a physician associate, a nurse or a specialist such as a physio, for example – could deal with just as well.
Advertisement
Hide AdAdvertisement
Hide AdDr Allen explained how it is decided which patients see GPs, and which are sent elsewhere for treatment.
Birley Medical Centre is one of two in Sheffield – along with Pitsmoor – which uses a tool called ‘askmyGP’ to manage all its appointments.
Patients get in touch either through the Birley Health Centre website, or by phoning up, and explaining their complaint. This is then entered into the askmyGP system where a member of staff who is doing the triaging – often the on-call doctor and a member of administrative staff – will assess it.
They then decide – based on things like who the patient has seen before and members of staff’s workloads – who can best deal with the issue at hand.
Advertisement
Hide AdAdvertisement
Hide AdDr Allen said: “Continuity is important. We always want people to see the same staff member when we can. If the last person they saw is not in, then we see if they can wait, and if they cannot we arrange for them to see somebody else.
“A patient will get in touch and often a receptionist will decide who is the best person a patient will see.”
When asked about patients becoming angry about an admin staff member deciding they should not see a GP straight away, Dr Allen said: "Our reception team have an excellent grasp of what kind of cases all our clinicians can see.
“They know who is in that day and they know what people are able to do.
Advertisement
Hide AdAdvertisement
Hide Ad“Patients can be sent to a PA or a nurse, but that does not mean that they will not at any point be seen by a GP.
“And, for example, if a PA feels like they need a GP to see a patient, they can refer them to one. Or they can have a patient come in and a GP can also go into the appointment as well.”
What is it like to be a GP at the moment?
In the past when The Star has spoken to GPs, some have suggested that the pressures of the job are causing some to reconsider their choice of career.
With the number of GPs in decline, this factor adds to the difficulties general practice already faces in the form of increased medical complexity and demand, and the lack of resources.
Advertisement
Hide AdAdvertisement
Hide AdDr Allen said: “It’s exhausting. When you see me you see a very different person at the end of each day compared to the start.
"But it is a privilege to support people who are ill, and patients on the whole are really pleased with the service they get here.
"Our workload has spiralled, medical complexity has spiralled and GP numbers are going down. That is why sometimes people can’t get appointments.
"I understand people being frustrated about that and we are doing our best.
Advertisement
Hide AdAdvertisement
Hide Ad“It is hard when the only time you get to reflect on the service the health centre provides, and how to improve it, is your time off, but that is what I have done and that is why I think we have done well.
"There needs to be changes, and I think general practice needs to better communicate these changes. We need to help patients to understand why we are working the way we are and show them the logic behind it.
“It is not as simple as somebody being ill and not being able to get an appointment. Most GPs are working really hard and they are exhausted and demoralised.
"Patients also need to be able to voice their anxieties so we can work together to improve the services GPs offer using systems that enable us to give people what they need."
